In addiction emergencies, clear and calm communication can save lives. Here’s what you need to know:
- Stay Calm: Panic can hinder your ability to act effectively. Observe symptoms like irregular breathing, unconsciousness, or blue skin.
- Use Trauma-Informed Language: Show empathy and respect. Avoid judgmental terms like “addict” and use person-first language (e.g., “person with a substance use disorder“).
- Follow the SCER Model:
- Self Check-In: Stay composed before acting.
- Clarify: Gather accurate details about the situation.
- Engage: Collaborate respectfully with the person in crisis.
- Resolve: Provide clear next steps, like calling 911 or administering naloxone.
- Communicate with 911: Be direct about symptoms (e.g., “not breathing”, “unconscious”) and share relevant details like substances involved or naloxone use.
- Prepare in Advance: Keep an emergency contact list and know how to use naloxone.
Overdose Prevention and Response in Crisis Care
Stay Calm and Assess the Situation
In an addiction emergency, staying composed is crucial. Your ability to remain calm directly impacts how effectively you can help. Panic clouds judgment and makes it harder to respond appropriately. The CDC’s Crisis + Emergency Risk Communication (CERC) framework advises responders to “Be right” and “Be credible” – and that begins with managing your own stress. Start by quickly evaluating the situation and identifying critical signs before taking further action.
Take a moment to observe. Look for key indicators such as unconsciousness or irregular breathing, like slow or gurgling breaths. Check for signs of oxygen deprivation, such as skin that appears blue, gray, or ashen, particularly around the lips or fingernails. The CDC highlights:
“It may be hard to tell whether a person is high or experiencing an overdose. If you aren’t sure, treat it like an overdose – you could save a life”.
Your emotional state also plays a significant role. Maintaining calm and demonstrating empathy can de-escalate the situation. Approaching someone in crisis with respect rather than judgment encourages cooperation and reduces the likelihood of defensive reactions. This emotional stability is key when applying Psychological First Aid (PFA), which helps stabilize both the environment and the person in distress.
Organize vital details immediately to ensure efficient communication with emergency responders. Note the symptoms you’re observing, the substances that might be involved, and your exact location. If possible, record this information for accuracy. For additional guidance, you can reach out to SAMHSA’s National Helpline at 1-800-662-HELP, which is available 24/7. Taking this structured approach not only helps you stay focused but also ensures you’re ready to provide clear information to emergency personnel.
Both overdose and withdrawal situations demand immediate professional care.
Use Trauma-Informed Communication Principles
In emergency response, using trauma-informed communication acknowledges that many individuals with substance use disorders have past trauma influencing their behavior during crises. This approach is built on four key principles: credibility, empathy, respect, and action. Applying these principles helps reduce conflict, fosters trust, and creates a foundation for effective intervention.
Understanding trauma patterns is critical. Defensive behavior, often mistaken for hostility, may actually be a protective response rooted in trauma. Responding with patience and understanding, rather than judgment, can help de-escalate situations and improve outcomes. Professionals who adopt trauma-informed methods often find their interventions more effective and less stressful for everyone involved. Below, we’ll explore how trauma impacts communication and how thoughtful language can build trust.
Understand How Trauma Affects Communication
Trauma shapes how individuals process information and respond to stress, especially during emergencies. For someone experiencing an addiction-related crisis, past trauma may cause them to misinterpret offers of help as threats. This can lead to defensive reactions, emotional withdrawal, or difficulty following instructions. Recognizing these behaviors as trauma responses, rather than intentional defiance, is key to adjusting your approach.
By understanding the root of these reactions, you can remain calm and maintain credibility. This shift allows you to respond thoughtfully, de-escalate tension, and focus on critical interventions that prioritize safety and care.
Avoid Stigmatizing Language
Language matters – stigmatizing terms can discourage people from seeking help and may trigger feelings of shame that shut down communication. According to the National Institute on Drug Abuse, stigma stems from misconceptions, such as the belief that individuals with substance use disorders are inherently dangerous or responsible for their condition.
Person-first language is a powerful tool for creating a more respectful and supportive environment. For example, instead of saying “addict” or “junkie”, use “person with a substance use disorder.” Similarly, replace terms like “clean” or “dirty” with “testing negative” or “testing positive” when discussing toxicology results. These changes emphasize that addiction is a chronic, treatable medical condition – not a moral failing.
| Instead of… | Use… | Why? |
|---|---|---|
| Addict, Junkie, User | Person with substance use disorder | Reduces negative stereotypes and avoids blame |
| Alcoholic, Drunk | Person with alcohol use disorder | Separates the person from their diagnosis |
| Habit, Choice | Substance use disorder, Disease | Avoids implying addiction is simply a matter of willpower |
| Clean / Dirty | Testing negative / Testing positive | Reframes language to avoid harmful moral judgments |
When initiating conversations, opt for non-judgmental openings like, “I notice you seem stressed, and I’m concerned”. Open-ended questions, such as “Can you tell me more about that?” encourage dialogue and give the individual a sense of control. Pam Lanhart, Founder and Director of Thrive Family Recovery Services, emphasizes the importance of listening:
“Just listen and be curious because they know what they need and will often come to the conclusion themselves”.
Use the Self Check-In, Clarify, Engage, Resolve (SCER) Model
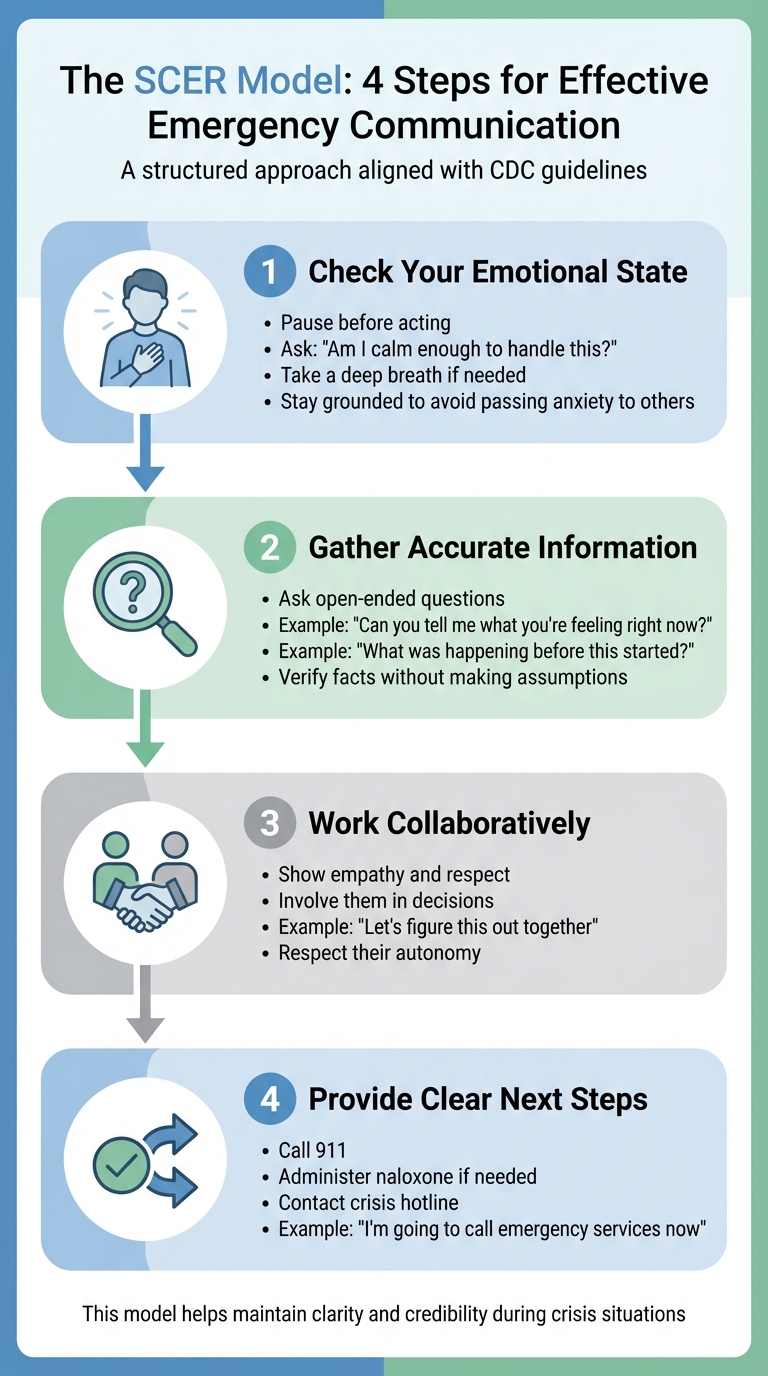
SCER Model for Addiction Emergency Communication
The SCER model offers a structured way to communicate during addiction emergencies. It aligns with CDC guidelines that focus on being clear, empathetic, and taking prompt action. By following these four steps, you can help bring clarity and guide the situation toward a solution.
Self Check-In
Before jumping into action, take a moment to check your emotional state. Stressful situations can lead to knee-jerk reactions that might escalate the problem. Pause and ask yourself: Am I calm enough to handle this? Do I need to take a deep breath before moving forward? This self-awareness helps you stay grounded, so you don’t unintentionally pass your anxiety onto the person in crisis. A calm demeanor is key to offering steady support.
Clarify the Problem
Take time to gather accurate information. Ask open-ended questions like, “Can you tell me what you’re feeling right now?” or “What was happening before this started?” These types of questions help you understand the situation without making assumptions. By verifying the facts, you maintain clarity and credibility in your communication.
Engage Collaboratively
Work with the person in crisis and anyone else present. Use language that shows empathy and respect, and involve them in decisions when possible. Instead of giving orders, try saying something like, “Let’s figure this out together. What do you think might help right now?” This approach respects their autonomy and keeps the focus on finding a safe solution.
Resolve with Options
Provide clear and actionable next steps. For instance, suggest calling 911, administering naloxone if an opioid overdose is suspected, or contacting a crisis hotline. Be direct and specific, using phrases like, “I’m going to call emergency services now so we can get help” or “Let’s reach out to someone who can assist us.” Outlining concrete actions ensures everyone knows what to expect and what needs to happen next. From here, you can focus on effectively communicating with emergency responders.
sbb-itb-17645e5
Deliver Clear Messages to Emergency Responders
When dealing with addiction-related emergencies, clear communication with 911 dispatchers is absolutely critical. The information you provide directly affects how quickly help arrives and whether the right type of assistance – police, fire, or EMS – is dispatched. Emergency responders rely on standardized questions to determine the situation’s severity and assign the proper medical priority. By sharing accurate, detailed information, you ensure that responders arrive prepared with the right equipment and knowledge to handle the situation.
Prepare Key Details in Advance
Planning ahead can make a huge difference in an emergency. Start by knowing your exact location – whether it’s your address or nearby landmarks – since relying solely on cellular data can sometimes lead to inaccuracies. Be ready to describe the person’s symptoms and have a record of any medications, allergies, or health conditions they might have.
Claire Zagorski, MSc, LP, a paramedic and researcher, offers this advice:
“My suggestion to people on the fence about calling 911 is to have a story ready to go in advance. You don’t need to mention the substances involved, but try to be specific about the symptoms the person is experiencing, like trouble breathing, loss of consciousness, or vomiting.”
If you carry naloxone, take the time to practice using it – whether it’s the nasal spray or the injectable vial. Being familiar with how it works can help you act quickly and confidently during a high-stress moment.
Communicate Effectively Under Pressure
When speaking to the dispatcher, describe the physical symptoms clearly and directly. Use phrases like “not breathing”, “unconscious”, “slow or ragged breathing”, or “vomiting.” These details help the dispatcher prioritize the call appropriately.
If the person is unresponsive, perform a sternum rub by rubbing their breastbone. If there’s no reaction, call 911 immediately and stay on the line to follow the dispatcher’s instructions.
Once EMS arrives, honesty becomes even more important. Zagorski stresses:
“This is when you’ll want to be as honest as possible about what happened, including the substances involved. This will help them determine the best course of action.”
If you’ve already administered naloxone, let the responders know how many doses were given and describe any reactions the person had. This information is vital for guiding their next steps.
Prepare an Emergency Contact List and Communication Protocols
Having a structured plan in place can make all the difference when time is critical. During a crisis, you don’t want to waste precious moments scrambling for contact information or figuring out who to notify first. Start by gathering all essential contacts, and then establish clear communication protocols.
Build a Comprehensive Contact List
Your emergency contact list should include key numbers like 911, the SAMHSA National Helpline at 1‑800‑662‑HELP (4357), and the 988 Suicide & Crisis Lifeline. Beyond these, make sure to add:
- Contact information for family members
- The individual’s primary physician or psychiatrist
- Addiction specialists
- Sponsors or counselors involved in their recovery
Include any relevant medical details, such as current medications, allergies, or a history of substance use. To ensure this information is accessible when needed, store it in a cloud-based or mobile-friendly format. Emergencies can happen anywhere, so having this data at your fingertips is crucial. Also, make it a habit to review and update the contact list regularly.
Establish Clear Communication Protocols
Define a clear notification process to maintain order during emergencies. For example, you might decide that 911 is always the first call, followed by a specific family member, and then the individual’s treatment provider. This ensures everyone is informed in the proper sequence.
Prepare template messages for common crisis scenarios like overdose or relapse. These pre-written messages can help you stay calm under pressure and convey vital information without hesitation. As Ron Derrick explains, “The way we control chaos during an emergency is through communication”. Assign specific roles to each person involved, so everyone knows exactly what to do when a crisis unfolds. Clear communication and defined roles can minimize confusion and make emergency responses more effective.
Conclusion
Handling an addiction emergency requires clear and effective communication to turn potential chaos into a coordinated response. The strategies outlined in this guide – remaining calm, using trauma-informed approaches, applying the SCER model, and preparing emergency protocols – combine to create a solid framework for navigating these challenging situations. As the CDC highlights, successful emergency response is anchored by six core principles: “1) Be first, 2) Be right, 3) Be credible, 4) Express empathy, 5) Promote action, 6) Show respect”.
Preparation plays a critical role. By setting up pre-scripted messages, maintaining updated emergency contacts, and establishing clear protocols, you can ensure that accurate information is delivered quickly. This groundwork allows you to focus entirely on the individual in crisis rather than scrambling for details when time is of the essence.
Empathy and respect are equally important. Using person-first language and steering clear of stigmatizing words fosters trust and cooperation. Approaching the situation with curiosity instead of judgment opens the door to honest conversations and meaningful steps forward. Together, these practices form a comprehensive and compassionate response to addiction emergencies.
A unified message ensures that every responder is aligned and ready to take life-saving action.
For more information on addiction recovery and treatment, visit Sober Living Centers.
FAQs
What is the SCER model, and how can it help during addiction emergencies?
The SCER model – short for Situational, Credibility, Empathy, and Response – is a framework crafted to guide communication during emergencies, including addiction-related crises. It focuses on understanding the scenario, establishing trust, demonstrating compassion, and providing clear, actionable guidance.
In the context of addiction emergencies, this model can help you approach the situation with focus and composure while addressing the immediate needs of those in distress. Here’s how it works:
- Situational: Start by assessing the circumstances to grasp what’s happening and identify what’s required.
- Credibility: Earn trust by sharing accurate, dependable information.
- Empathy: Express genuine care and understanding for the individual’s emotions and challenges.
- Response: Offer clear, actionable steps, such as contacting medical professionals or exploring treatment options.
Applying the SCER model helps minimize confusion and panic, paving the way for effective decision-making. In high-pressure moments, like overdoses or withdrawal episodes, staying composed, compassionate, and clear can make all the difference in steering the situation toward a better outcome.
How can trauma-informed communication help during addiction emergencies?
Trauma-informed communication can play a crucial role during addiction emergencies by fostering a safe and supportive environment for those in distress. Instead of asking, “What’s wrong with you?”, this approach shifts the focus to “What happened to you?”. This subtle yet powerful change acknowledges the impact of past trauma and avoids actions that might unintentionally cause further harm.
By emphasizing empathy, respect, and clear communication, this method helps to build trust, ease anxiety, and encourage cooperation. It’s not just about managing the immediate crisis – it’s about understanding the person’s emotional state and history. This approach can de-escalate tense situations and create a foundation for better engagement, ultimately supporting both immediate relief and long-term recovery.
Why is it important to use person-first language during addiction emergencies?
Using person-first language during addiction emergencies plays a crucial role in fostering understanding and reducing stigma. This approach puts the individual before their condition, emphasizing their humanity and preserving their dignity. For instance, referring to someone as “a person with a substance use disorder” instead of “an addict” highlights that addiction is just one aspect of their life, not their entire identity.
Studies have shown that stigmatizing language can discourage people from seeking help and may even influence how healthcare providers interact with them. By choosing respectful and non-judgmental terms, we can create a more compassionate environment that supports recovery and makes it easier for individuals to access the care they need. These small shifts in language can have a profound impact on breaking down barriers and encouraging healing.


