Polysubstance use, or mixing multiple drugs, significantly raises overdose risks due to unpredictable and amplified effects. In 2022, nearly half of all overdose deaths involved multiple substances, with synthetic opioids like fentanyl often mixed with stimulants or depressants, sometimes unknowingly. Contaminated drugs, like counterfeit pills laced with fentanyl or xylazine, further complicate the crisis, making overdoses harder to treat and more fatal.
Key points:
- Mixing drugs multiplies risks: Combining stimulants and depressants masks symptoms, leading to higher consumption and increased toxicity.
- Drug contamination is widespread: In 2023, 93% of fentanyl-positive samples contained other substances.
- Young people are at high risk: Counterfeit pills and hidden drug combinations disproportionately affect younger users.
- Naloxone remains critical: While helpful for opioid overdoses, it may not reverse effects of contaminants like xylazine.
Understanding these dangers and improving access to harm reduction tools, treatment, and education can save lives.
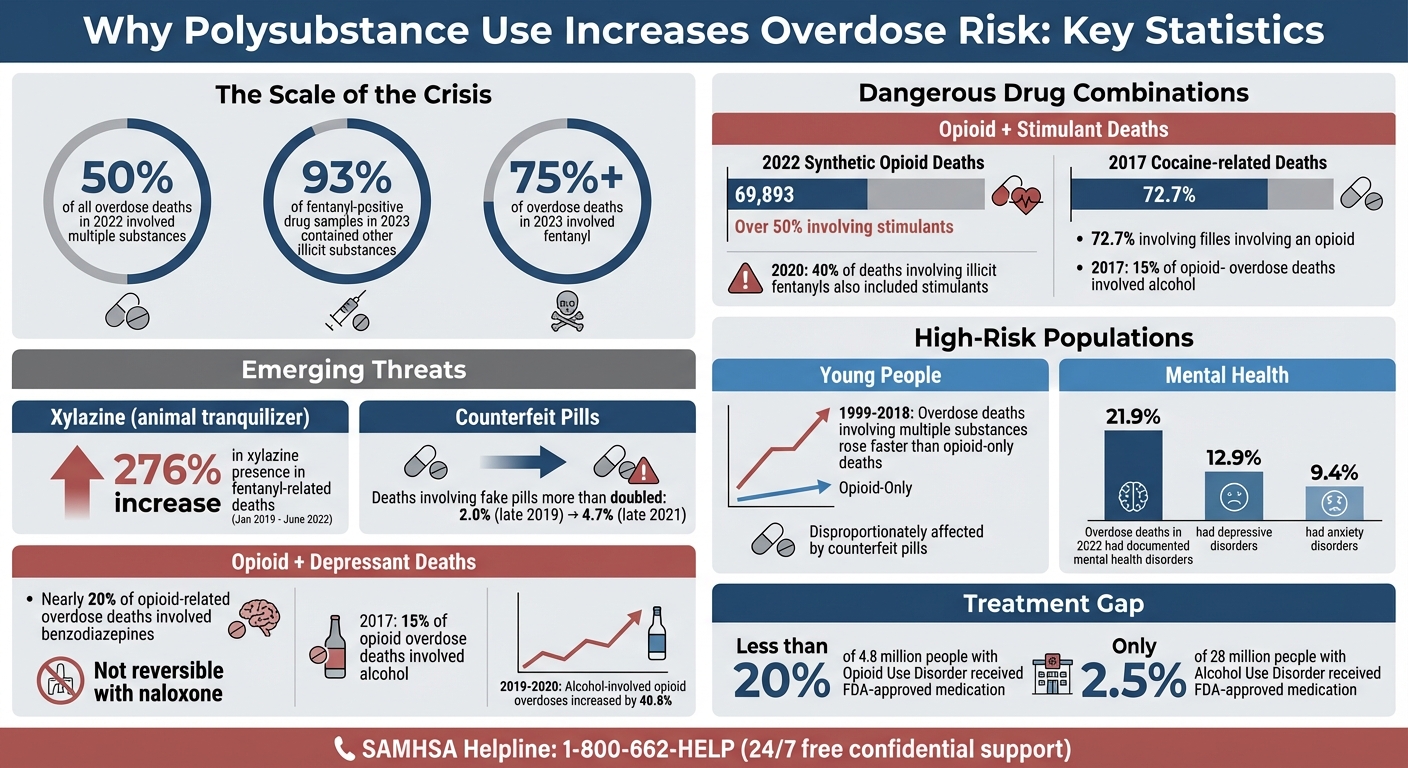
Polysubstance Use Overdose Statistics and Risk Factors
Research Into Action: Polysubstance Use: Methamphetamine Amidst the Overdose Crisis
sbb-itb-17645e5
What Is Polysubstance Use?
Polysubstance use involves taking multiple drugs either at the same time or one after another. Sometimes this is done on purpose – to heighten a high, reduce unwanted effects, or achieve a particular feeling. Other times, it happens unknowingly, such as when a drug is contaminated with substances like fentanyl or xylazine. Grasping the dynamics of this behavior is essential for tackling the overdose crisis explored in this article.
A common misconception is that combining stimulants and depressants cancels out their effects. In reality, they mask each other, leading users to take more and significantly increasing the risk of overdose. Adding to the danger, drug contamination further complicates the issue.
How Fentanyl Contamination Drives Polysubstance Use
Polysubstance use isn’t always intentional; contamination plays a major role. In 2023, 93% of fentanyl-positive drug samples were found to contain other illicit substances. This means someone buying what they think is a single drug – like cocaine, methamphetamine, or a prescription pill – could unknowingly be exposed to a dangerous mix.
Drug traffickers intentionally add fentanyl to non-opioid drugs to make them more addictive. Dr. Lantie Elisabeth Jorandby, Chief Medical Officer at Lakeview Health, explains:
Illicit drug manufacturers and dealers do this to get their customers hooked so they come back for more. For them, it’s a sales tactic.
The problem doesn’t stop there. From January 2019 to June 2022, xylazine’s presence in fentanyl-related deaths surged by 276%. Xylazine, a veterinary tranquilizer not meant for humans, is now frequently found in drug supplies. Counterfeit pills are another growing threat – overdose deaths involving fake pills more than doubled, rising from 2.0% in late 2019 to 4.7% by late 2021.
Polysubstance Use Statistics
The numbers paint a grim picture. By 2023, fentanyl was involved in over 75% of overdose deaths, and many of these also included stimulants like cocaine or methamphetamine. This trend has become so widespread that experts now describe it as the “fourth wave” of the overdose crisis.
Benzodiazepines were found in nearly 20% of opioid-related overdose deaths. In 2022, more than half of the 69,893 synthetic opioid overdose deaths involved stimulants. These shifts highlight how mixing drugs creates unpredictable and often deadly risks, underscoring the need for comprehensive prevention and treatment efforts.
Why Polysubstance Use Increases Overdose Risk
Mixing drugs doesn’t just add risks – it multiplies them. In 2022, half of all overdose deaths involved multiple substances. Combining different drugs can create dangerous physiological conflicts that single substances alone don’t cause, making overdoses both more frequent and harder to treat.
One particularly risky misconception is that mixing stimulants and depressants balances their effects. According to the CDC:
Mixing stimulants and depressants doesn’t balance or cancel them out. In fact, the results of combining drugs are unpredictable, often modifying or even masking the effects of one or both drugs.
This masking effect can trick users into consuming more than they realize, putting them at greater risk. In 2016, nearly 80% of synthetic opioid-related overdose deaths involved at least one other substance. When opioids and stimulants are used together, the body faces a deadly contradiction: opioids slow breathing, while stimulants increase oxygen demand on the heart. This combination can lead to fatal cardiac arrhythmias.
Depressants, when combined, are just as deadly. Pairing opioids with alcohol or benzodiazepines – both of which suppress the central nervous system – intensifies respiratory depression. As the Pew Charitable Trusts explains:
Opioid use concurrent with the use of another sedating drug compounds the respiratory depressant effect of each drug, creating a higher risk for overdose and fatal overdose than when either drug is used alone.
In 2017, 15% of opioid overdose deaths involved alcohol, and between 2019 and 2020, alcohol-involved opioid overdoses increased by 40.8%. These interactions magnify harm, making the outcome far worse than with any single substance.
How Drug Combinations Increase Toxicity
When drugs interact, their combined effects often exceed the sum of their individual risks. For example, combining multiple depressants doesn’t just add their effects – it multiplies them, pushing the body beyond critical thresholds. In the first half of 2018, nearly 63% of opioid overdose deaths involved substances like cocaine, methamphetamine, or benzodiazepines.
Stimulant-opioid combinations are particularly dangerous. Stimulants can mask opioid sedation, leading users to take higher, potentially fatal doses without recognizing the warning signs. Meanwhile, respiratory depression caused by opioids remains untreated. In 2017, 72.7% of cocaine-related overdose deaths also involved an opioid, and by 2020, 40% of deaths involving illicit fentanyls also included stimulants.
Contamination further amplifies these dangers. Many users unknowingly take drugs laced with substances like fentanyl, for which they have no tolerance. In 2022, over 50% of the 69,893 synthetic opioid overdose deaths also involved stimulants. The presence of xylazine, an animal tranquilizer that naloxone cannot reverse, has added another layer of risk. These factors create a deadly landscape, especially for younger users.
Rising Overdose Rates Among Young People
Young people face unique risks from polysubstance use, particularly due to counterfeit pills. Between 1999 and 2018, overdose deaths among young people involving multiple substances rose faster than those involving opioids alone. Counterfeit pills, often containing hidden combinations of drugs like fentanyl, drive this trend.
The statistics are alarming. Overdose deaths linked to counterfeit pills more than doubled, rising from 2.0% in late 2019 to 4.7% by late 2021. Younger individuals, especially those who are Hispanic and have a history of prescription drug misuse, are at greater risk. With little to no tolerance for potent synthetic opioids hidden in these pills, even a single dose can be lethal.
In a 2025 study, researchers led by Eduardo R. Butelman, PhD, at the Icahn School of Medicine at Mount Sinai, analyzed CDC data from 2018–2024. They found that while polydrug overdose mortality involving synthetic opioids and stimulants decreased significantly in 2024 compared to 2023 – showing an annual decline of 36% in males and 31% in females – mortality rates remain troublingly high.
Single-Substance vs. Polysubstance Overdose Comparison
To understand why combining drugs is so dangerous, it’s helpful to compare the risks of single-substance overdoses with those of polysubstance use. The table below highlights key differences:
| Overdose Type | Primary Risk Factors | Physiological Impact | Predictability |
|---|---|---|---|
| Single-Substance (Opioid) | High potency (e.g., fentanyl), low tolerance | Severe respiratory depression and failure | Effects generally align with the drug class |
| Single-Substance (Stimulant) | Cardiovascular strain, high dosage | Heart attack, stroke, or neurological damage | Predictable physiological effects |
| Polysubstance (Opioid + Alcohol) | Combined depressant effects | Multiplied respiratory depression; brain and heart damage | Highly unpredictable; effects multiply |
| Polysubstance (Opioid + Stimulant) | Masked symptoms, unpredictable toxicity | Cardiac arrhythmia from oxygen demand vs. hypoxia | Substances mask each other’s effects |
| Polysubstance (Opioid + Benzodiazepines) | Dual depressant action | Extreme respiratory failure risk | Multiple failure points |
The takeaway is clear: single-substance overdoses follow more predictable patterns, while polysubstance use introduces chaotic, often deadly interactions. Hidden contaminants, like fentanyl, eliminate any margin for error.
What Causes Polysubstance Overdose Deaths
Polysubstance overdose deaths are not simply the result of individual decisions. A mix of economic hardship, mental health issues, and the constantly shifting drug landscape creates the conditions for these tragedies. Key contributors include counterfeit drugs, mental health struggles, and the emergence of new substances, all of which play a role in the rising number of fatalities.
Counterfeit Pills and Stronger Drugs
The illicit drug market is driven by profit, often at the expense of safety. Counterfeit pills laced with fentanyl are a prime example. According to Dr. Lantie Jorandby, Chief Medical Officer:
Illicit drug manufacturers and dealers do this to get their customers hooked so they come back for more. For them, it’s a sales tactic.
These counterfeit pills are designed to mimic legitimate medications like oxycodone (M-30) or alprazolam (Xanax) but frequently contain dangerous substances like illicitly manufactured fentanyls or benzodiazepines. Social media platforms have become a hub for selling these counterfeits, often targeting younger individuals who may have little to no drug tolerance. The problem is especially severe in certain regions. For instance, between 2019 and 2021, the western U.S. saw a threefold increase in counterfeit pill evidence, with 55.8% of overdose deaths in this area involving these pills, compared to just 16.3% in other regions.
Mental Health and Substance Use
Mental health issues significantly increase the risk of overdose. In 2022, 21.9% of people who died from drug overdoses had a documented mental health disorder. The most common were depressive disorders (12.9%), anxiety disorders (9.4%), and bipolar disorders (5.9%). Many individuals turn to substances to self-medicate or manage symptoms, which becomes especially risky when prescription medications are involved. For example, overdose deaths involving benzodiazepines and antidepressants were significantly higher among those with mental health disorders – 15.3% and 9.7%, respectively – compared to those without.
Stigma and systemic gaps in care often prevent people from getting the help they need. Integrated treatment facilities that address both mental health and addiction are scarce, leaving many without proper support. Additionally, access to life-saving medications remains limited. In 2024, fewer than 20% of the 4.8 million individuals with Opioid Use Disorder received any FDA-approved medication due to economic and regulatory barriers.
New Drugs Entering the Market
The introduction of new drugs adds another layer of complexity. Xylazine, an animal tranquilizer, has become a particularly dangerous addition to the drug supply. Its involvement in fentanyl-related deaths skyrocketed by 276% between January 2019 and June 2022. Unlike opioids, xylazine does not respond to naloxone, making overdose reversals far more challenging.
Unpredictable drug combinations further heighten overdose risks. A common misconception is that mixing stimulants and depressants “balances out” their effects, a practice sometimes referred to as “goofballing.” In reality, this combination is extremely hazardous. Instead of neutralizing each other, these substances can mask overdose symptoms, leading users to consume more than is safe.
Rural areas face unique challenges in addressing these dangers. Long distances to healthcare facilities, limited provider availability, and financial barriers make accessing care even harder. These factors illustrate why polysubstance use continues to drive overdose deaths. Understanding these causes is crucial for developing effective harm reduction and treatment strategies, which will be explored next.
How to Reduce Polysubstance Overdose Risks
Lowering the risks associated with polysubstance overdoses requires both immediate harm reduction techniques and long-term treatment plans. The focus should first be on ensuring safety and then on addressing the root causes of substance use with proven, evidence-based care.
Harm Reduction Methods
Naloxone is a lifesaving tool for reversing opioid overdoses, even in cases where other substances are involved. As of 2023, naloxone is available over the counter in intranasal forms, making it more accessible than ever. For suspected opioid overdoses, administer naloxone at 0.4 mg intramuscularly or 3.0–4.0 mg intranasally. Dr. Kelly S. Ramsey, MD, an expert in addiction medicine and harm reduction, advises:
While a person may still be unconscious, additional naloxone is not needed if regular breathing is restored.
After giving the first dose, wait 2–3 minutes to see if breathing resumes before administering a second dose. If the person is breathing but unresponsive, placing them in the recovery position can help prevent choking while waiting for emergency responders.
Drug checking is another vital harm reduction tool, especially given the unpredictable nature of the illicit drug supply. Fentanyl and xylazine test strips allow users to detect harmful additives in substances like pills, powders, and injectables. This is especially important for those primarily using stimulants, as they may not carry naloxone.
While these interventions are crucial in the moment, addressing long-term risks requires a shift toward comprehensive treatment.
Treatment Options for Polysubstance Use
Harm reduction is just the first step. Effective treatment should address underlying substance use disorders. Medications for Opioid Use Disorder (MOUD), such as buprenorphine and methadone, have been shown to significantly lower overdose deaths. Quick access to these medications – through bridge clinics or emergency department programs – can reduce barriers to care. Importantly, MOUD remains effective even when combined with stimulant use, and stopping MOUD can increase the risk of overdose.
For stimulant use disorders, there are no FDA-approved medications, making behavioral therapies like contingency management critical. This approach incentivizes negative drug tests with monetary rewards and is considered the standard for treating cocaine and methamphetamine use. Some states fund these programs through Medicaid waivers, and the Veterans Health Administration has long used contingency management as a successful model.
Given the prevalence of combined substance use, treatment plans must address multiple substances simultaneously.
Getting Comprehensive Care
Early intervention is key to saving lives, but systemic barriers often delay or prevent access to care. For example, prior authorization requirements, mandatory counseling, and daily clinic visits for methadone can create unnecessary hurdles. In 2024, fewer than 20% of the 4.8 million individuals with Opioid Use Disorder received any FDA-approved medication.
Some states are exploring innovative funding models to address these challenges. Michigan and Massachusetts, for instance, use fixed monthly rates and block grants to ensure providers can deliver uninterrupted, comprehensive care.
Programs should also eliminate “administrative discharge”, a practice where patients are removed from care for continued substance use. Instead, care levels should be adjusted to keep individuals engaged. Medicaid managed care organizations can further support recovery by covering all FDA-approved medications for Opioid Use Disorder and Alcohol Use Disorder without prior authorization. This is particularly important, as 23% of individuals with opioid use disorder also have a co-occurring alcohol use disorder.
By integrating harm reduction with tailored treatment plans, a continuum of care can be established, significantly reducing the risks of polysubstance overdoses.
For additional resources, Sober Living Centers (https://soberlivingcenters.com) offers information on treatment options and can help locate rehab facilities equipped to address multiple substance use issues.
Resources for Recovery and Overdose Prevention
Getting the right support can make all the difference when it comes to minimizing the risks of polysubstance use. Across the U.S., there are national and community-based resources offering immediate help, educational tools, and connections to treatment. Below, you’ll find key information on educational materials and services that can guide you toward effective treatment and harm reduction strategies.
Educational Materials on Addiction
Understanding the dangers of polysubstance use is a critical step in prevention. One resource to know is SAMHSA‘s National Helpline (1-800-662-HELP), a free, confidential service available 24/7 in both English and Spanish. In 2020 alone, this helpline received 833,598 calls, marking a 27% increase from the year before. Another helpful tool is the CDC Overdose Resource Exchange (ORE), which offers a wide range of educational materials focused on opioid misuse, addiction treatment, and prevention strategies.
For more detailed insights, Sober Living Centers (https://soberlivingcenters.com) provides resources that break down the effects, causes, and symptoms of polysubstance use. Their evidence-based guides emphasize the risks of mixing substances – a critical topic, as nearly half of all overdose deaths in 2022 involved multiple drugs. These materials also help identify warning signs like mood swings and memory blackouts, while offering prevention tips and treatment options.
Finding Treatment Centers and Support
Once you understand the risks, finding the right treatment becomes the next crucial step. Access to specialized care can significantly reduce the dangers of polysubstance use. SAMHSA’s online locator and text service (text your ZIP code to 435748) make it easy to find nearby rehab centers and support groups. For those without insurance, SAMHSA can also connect you to state-funded programs or facilities that accept Medicare, Medicaid, or offer sliding fee scales.
Sober Living Centers is another excellent resource for connecting individuals to professional treatment options tailored to address both substance use and co-occurring mental health conditions. This is especially important since mental health struggles often increase the risk of polysubstance overdose. Additionally, the National Harm Reduction Coalition (harmreduction.org) provides tools for finding local naloxone distribution sites, syringe service programs, and overdose prevention tips.
Conclusion
Polysubstance use is at the heart of today’s overdose crisis. In 2022, nearly half of all drug overdose deaths involved multiple substances. The danger lies in the unpredictability of combining drugs, which can amplify effects and lead to fatal outcomes. As Shannon Cassius, an epidemiologist at the CDC, warns:
Whether intentional or not, mixing drugs is never safe because the effects from combining drugs may be stronger and more unpredictable than one drug alone, and even deadly.
While harm reduction tools like naloxone and drug-checking strips are critical, they’re not enough on their own. Effective treatment must tackle the broader challenges of polysubstance use, including co-occurring mental health issues and the use of FDA-approved medications for opioid and alcohol use disorders. However, these solutions can only make a difference if access to care improves.
Right now, access remains a major barrier. In 2024, fewer than 20% of the 4.8 million people with opioid use disorder and only 2.5% of the nearly 28 million individuals with alcohol use disorder received FDA-approved medications. This gap in care has deadly consequences, especially as lost tolerance during abstinence significantly raises the risk of relapse. These statistics highlight the complexity of the crisis and the pressing need for comprehensive, integrated approaches.
FAQs
What are the most dangerous drug combinations?
The riskiest drug combinations include mixing alcohol with opioids or benzodiazepines, cocaine with heroin, and alcohol with cocaine. These pairings dramatically heighten the chances of overdose because of their dangerous interactions and amplified effects. Recognizing these dangers is key to prevention and reducing harm.
How can I tell if a pill or powder is contaminated?
To determine if a pill or powder is tainted, you can use fentanyl test strips to identify the presence of fentanyl or related synthetic opioids. These substances are often found in street drugs and significantly raise the risk of overdose. Testing what you plan to use beforehand can help lower this risk.
What should I do if naloxone doesn’t wake someone up?
If naloxone doesn’t work, call 911 immediately. You can give more doses of naloxone if you have them, while keeping a close eye on their breathing and airway. Stay by their side to ensure they’re safe until emergency responders arrive.


