Addiction recovery often impacts more than just mental health – it can weaken your bones too. Alcohol, opioids, and other substances disrupt bone-building cells, lower essential hormones, and deplete critical nutrients like calcium and vitamin D. Ignoring these effects increases the risk of osteoporosis, fractures, and long-term damage.
Key Takeaways:
- Substance Effects: Alcohol suppresses bone formation, while opioids and methamphetamine lead to low bone density and osteoporosis.
- Nutrition Matters: Poor diets linked to addiction worsen bone health by reducing calcium, vitamin D, and magnesium levels.
- Exercise Helps: Weight-bearing and strength-training exercises stimulate bone growth and reduce fracture risks.
- Quitting Alcohol/Tobacco: Stopping substance use can improve bone formation in just weeks.
- Medical Support: Regular bone density scans and monitoring can track recovery progress.
Recovery Tip: Pair a nutrient-rich diet (1,000–1,200 mg calcium and 600–800 IU vitamin D daily) with moderate exercise to rebuild strength. Consult your doctor for personalized care, especially if you’ve experienced fractures or have low bone density.
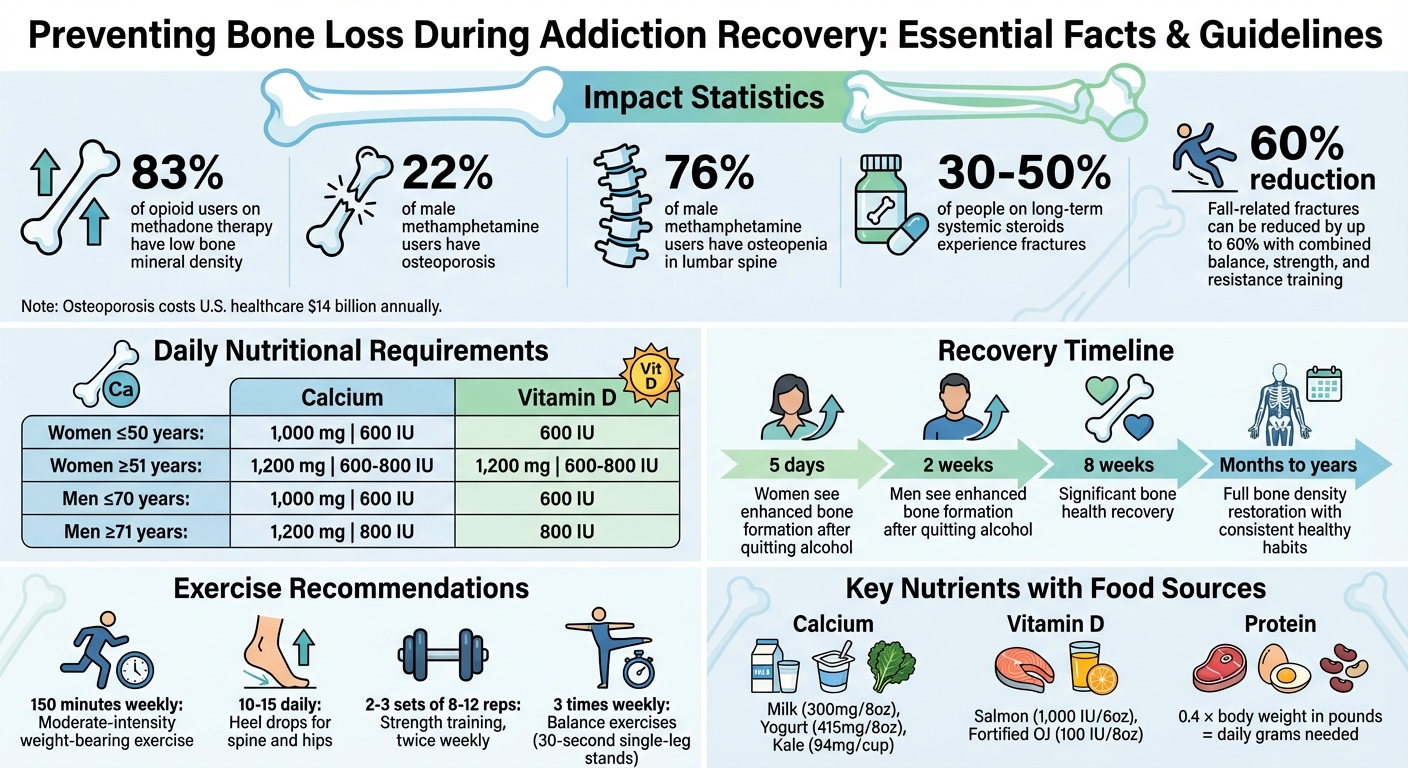
Addiction’s Impact on Bone Health: Key Statistics and Recovery Guidelines
How Addiction Damages Bone Health
How Substance Abuse Weakens Bones
Addiction takes a serious toll on the skeletal system, making recovery even more challenging. Substances like alcohol and opioids suppress osteoblast activity – the cells responsible for building bone – leading to reduced bone formation. Long-term substance use also disrupts the hypothalamic-pituitary-gonadal axis, which can result in hypogonadism. This condition causes lower testosterone levels in men and reduced estrogen levels in women, both of which are critical for maintaining bone mass. Studies reveal alarming statistics: 83% of opioid users undergoing methadone therapy have low bone mineral density, while male methamphetamine users show a 22% rate of osteoporosis and a 76% rate of osteopenia in the lumbar spine.
“Alcohol appears to suppress osteoblast function in adults, resulting in decreased bone formation.” – H. Wayne Sampson, Ph.D., Professor, Texas A&M Health Science Center
Other substances also wreak havoc on bone health. Tobacco and THC from cannabis activate cellular pathways that increase bone breakdown. Methamphetamine, on the other hand, disrupts stem cell maturation, preventing these cells from becoming bone-forming osteoblasts. Intravenous drug use adds another layer of risk by increasing the chance of developing osteomyelitis – a severe bone infection that can cause lasting skeletal damage.
Addiction’s impact on bone health isn’t limited to cellular damage. Poor nutrition, often a byproduct of substance abuse, further weakens the bones.
How Poor Nutrition Affects Bone Strength
Nutritional deficiencies caused by addiction amplify the damage to bone health. Alcohol, for instance, interferes with calcium and vitamin D absorption in the small intestine. It also disrupts the liver and kidneys’ ability to convert vitamin D into its active form, making it harder for the body to utilize these essential nutrients – even with a balanced diet.
Substance abuse often leads to poor eating habits that further harm bone health. Stimulants like cocaine and methamphetamine suppress appetite, leading users to skip meals or choose unhealthy, calorie-dense foods over nutrient-rich options. This diet pattern can deplete vitamin C levels, which are crucial for collagen production and joint repair. Additionally, poor nutrition can impair the production of insulin-like growth factor 1 (IGF-1) and disrupt parathyroid hormone function, both of which are essential for bone remodeling and calcium balance.
Addressing these nutritional deficiencies is a key step in preventing further bone damage during recovery. Together, these factors highlight the critical need for comprehensive strategies to protect bone health in individuals struggling with addiction.
sbb-itb-17645e5
Exercise Strategies to Prevent Bone Loss
Weight-Bearing Exercises
Engaging in regular weight-bearing activities is a key way to rebuild bone strength, especially during addiction recovery. These exercises – where you work against gravity while remaining upright – help activate osteoblasts, the cells responsible for creating new bone tissue. When paired with abstinence, these activities can speed up bone health recovery by addressing the imbalance between bone breakdown and formation.
“The initial imbalance between bone formation and resorption seems to straighten out during abstinence. This means that an increased fracture risk could be reduced during abstinence if no manifest osteoporosis is already present.” – Peter Malik, Senior Scientist and Physician, Medical University Innsbruck
Brisk walking is a great place to start. Aim for a pace of 3 to 4 miles per hour, as slower speeds may not provide enough stimulation for bone growth. If you’re dealing with significant bone loss, low-impact options like an elliptical machine or fast walking on a treadmill can be safer alternatives. To further boost bone health, consider using a weighted vest set to about 5% of your body weight. Aim for at least 150 minutes of moderate-intensity weight-bearing exercise weekly, and include 10 to 15 heel drops daily to gently target your spine and hips. Adding resistance and balance exercises to your routine can complement these efforts and strengthen bones even more.
Strength Training and Balance Exercises
In addition to weight-bearing exercises, strength and balance training are crucial for improving bone health during recovery. Resistance training, which involves muscle contractions, encourages osteoblast activity to rebuild bone, following the principles of Wolff’s Law. Begin with simple bodyweight exercises like sit-to-stand movements, wall push-ups, or bridges. Perform 8 to 12 repetitions for 2 to 3 sets, twice a week. Once you’ve mastered the basics, gradually introduce light weights (2 to 5 lbs) or resistance bands. If you don’t have access to gym equipment, household items like water bottles can work as substitutes.
Balance exercises are just as important because falls often lead to fractures. Combining balance, strength, and resistance training has been shown to reduce fall-related fractures by up to 60%. Try exercises like tandem stance (heel-to-toe walking), single-leg stands for 30 seconds on each side, or even Tai Chi movements, practicing at least three times a week. Keep a sturdy chair or countertop nearby for support as you build your confidence. Avoid high-impact or overly strenuous exercises that could stress weakened bones. Before starting any new routine, especially if you’ve had fractures in the past, consult your doctor. Progress slowly by increasing either the weight or the number of repetitions, but never both at the same time.
Nutrition Strategies for Bone Health
Key Nutrients for Strong Bones
A nutrient-packed diet is just as important as exercise when it comes to rebuilding bone health, especially during recovery. To address bone loss, focus on specific nutrients that help strengthen and maintain your bones.
Calcium and vitamin D are a dynamic duo for bone health. Calcium builds the mineral foundation needed for strong bones, while vitamin D ensures your body can absorb and use that calcium effectively. Without enough vitamin D, even a diet high in calcium won’t provide the benefits your bones need.
You can find calcium in dairy products like milk (300 mg per 8-ounce glass), yogurt (415 mg per 8-ounce serving), and cheese. If you prefer non-dairy options, fortified plant-based milks and leafy greens like kale (94 mg per cup) are great alternatives. For vitamin D, include fatty fish like salmon (1,000 IU per 6-ounce serving), fortified orange juice (100 IU per 8 ounces), and egg yolks in your diet.
Other important nutrients include magnesium and phosphorus, which heavy alcohol consumption can deplete. These minerals are critical for maintaining bone structure. Replenish them by adding foods like spinach, almonds, and avocados to your meals.
Daily Nutritional Requirements Table
The amount of calcium and vitamin D your body needs changes with age and gender. Women over 51 and men over 71 generally require higher amounts to counteract natural bone loss.
| Life Stage / Group | Daily Calcium | Daily Vitamin D |
|---|---|---|
| Women ≤ 50 years | 1,000 mg | 600 IU |
| Women ≥ 51 years | 1,200 mg | 600–800 IU |
| Men ≤ 70 years | 1,000 mg | 600 IU |
| Men ≥ 71 years | 1,200 mg | 800 IU |
For better calcium absorption, spread your intake across smaller doses (500–600 mg) throughout the day. For example, if you need 1,200 mg daily, divide it into two or three portions with meals. A quick tip: to estimate calcium content from a nutrition label, just add a zero to the “Percent Daily Value” listed. For instance, 25% Daily Value equals about 250 mg of calcium.
Protein is another essential component of bone health, as it plays a major role in rebuilding bone tissue.
How Protein Supports Bone Health
Protein makes up about 50% of your bone structure, acting as a framework where calcium and phosphorus are deposited. Dr. Harold Rosen, Director of the Osteoporosis Prevention and Treatment Center at Beth Israel Deaconess Medical Center, describes it clearly:
“Protein is like scaffolding. Calcium and phosphorous form on it and stiffen up”.
Without enough protein, your body struggles to repair bone tissue and rebuild strength during recovery.
To calculate your daily protein needs, multiply your body weight in pounds by 0.4. For instance, a 140-pound individual would need about 56 grams of protein daily to support bone health. Great protein sources include lean meats, poultry, fish, eggs, beans, and Greek yogurt. Foods like canned salmon with bones, sardines, and dairy products offer the added bonus of both protein and calcium. Distributing your protein intake evenly across meals can also help ensure steady tissue repair throughout the day.
Lifestyle Adjustments and Medical Monitoring
Quitting Alcohol and Tobacco
Stopping alcohol and tobacco use is the most critical step for protecting your bones during recovery. Quitting alcohol leads to noticeable improvements in bone health fairly quickly – women often see enhanced bone formation within 5 days, while men typically notice changes within 2 weeks. Significant recovery can occur within about 8 weeks.
Tobacco use, on the other hand, disrupts the activity of bone-building cells and speeds up estrogen breakdown in women, which accelerates bone loss. When combined, alcohol and tobacco create a double threat, making it much harder for bones to heal and rebuild. Giving up these substances helps restore the balance between bone breakdown and formation that addiction disrupts.
Getting Regular Bone Density Scans
Once you’ve stopped using alcohol and tobacco and slowed bone loss, regular monitoring becomes key. A DXA (Dual-energy X-ray absorptiometry) scan is an effective tool for assessing bone health. It measures bone mineral density and provides a T-score that compares your bone strength to that of a healthy 30-year-old. If you’ve had a history of heavy substance use, scheduling a baseline DXA scan is a smart first step to track your progress.
The frequency of follow-up scans depends on your results. For osteopenia (low bone mass), scans every 1–2 years are typical, while osteoporosis usually requires annual monitoring. To ensure consistent results, it’s best to stick with the same facility for all scans. Keep in mind, you should avoid taking calcium supplements 24 hours before the scan to maintain accuracy. Without insurance, a DXA scan generally costs between $300 and $500.
Working with Healthcare Providers
In addition to quitting harmful substances and monitoring bone density, partnering with healthcare providers is essential for managing your bone health. Regularly reviewing your prescriptions is critical, as some medications – like corticosteroids, SSRIs, and anticonvulsants – can accelerate bone loss. Studies show that 30% to 50% of people on long-term systemic steroids may experience fractures as a result.
Medical monitoring also helps address the broader effects of substance abuse on the body. Damage to the endocrine system, liver, and pancreas can interfere with vitamin D activation, calcium absorption, and hormone regulation, all of which are vital for maintaining strong bones. Blood tests can reveal deficiencies in nutrients like vitamin D, B12, and folic acid, allowing doctors to create a personalized treatment plan. Collaborating with an interdisciplinary team – including physicians, nurses, and physical therapists – ensures that both your recovery and bone health are supported. This integrated approach strengthens your skeletal system while helping you stay on track in your recovery journey.
For more resources on addiction recovery and overall wellness, check out the educational materials available through Sober Living Centers.
Alcohol REDUCES BONE HEALTH! – #sober #sobercurious #sobriety #osteoporosis #bonehealth
Conclusion
Focusing on recovery strategies that include exercise, nutrition, and lifestyle changes is key to regaining mobility and promoting long-term health. Recovery is especially important for bone health, as addiction can weaken bones and lower mineral density, increasing the risk of fractures. By quitting substances and adopting targeted nutrition and exercise routines, you can start reversing bone damage within days to weeks, with noticeable improvements often appearing after about eight weeks.
“The application of scientifically based methods to support and stimulate long-term recovery processes in post-withdrawal alcoholics can dramatically improve quality of life and rehabilitation success” – Sergei Mechtcheriakov, Associate Professor of Psychiatry, Medical University Innsbruck
To protect your bones, begin with these essential steps: stop using alcohol and tobacco, incorporate weight-bearing exercises into your routine, and ensure your diet includes 1,000–1,500 mg of calcium and 400–800 IU of vitamin D daily. It’s also a good idea to schedule a DEXA scan to assess your baseline bone density and consult with your healthcare provider about any medications that might impact your bone health. Keep in mind that osteoporosis, often called a “silent disease”, can progress unnoticed for years until a fracture occurs – making proactive care essential.
While full restoration of bone density can take months or even years of consistent healthy habits, the effort is worth it. Preventing osteoporotic fractures not only protects your mobility and independence but also saves the U.S. healthcare system approximately $14 billion annually.
For more evidence-based tips and resources on recovery and bone health, visit Sober Living Centers.
FAQs
Do I need a DXA scan during recovery?
A DXA scan is a simple and painless way to check your bone health and catch early signs of osteoporosis. Whether you need one during your recovery depends on your individual health situation and risk factors, like heavy alcohol consumption or medical conditions that impact your bones. If you’re worried about bone loss or osteoporosis, talk to your healthcare provider to see if a DXA scan makes sense for you.
Can my bones recover after I quit drinking or opioids?
Yes, your bones can regain strength after you stop using alcohol or opioids, though the degree of recovery depends on how long and how severely they were affected. Quitting, along with a diet rich in calcium and vitamin D and regular physical activity, plays a key role in supporting bone health. While some long-term damage might not fully reverse, your body has an impressive ability to repair and rebuild bone tissue over time when given the right care.
Which supplements are safe to take in recovery?
Safe supplements during recovery often target areas like brain health, detox support, and bone strength. Citicoline is known to potentially boost cognitive function, making it a helpful option for mental clarity. N-Acetyl Cysteine (NAC) can assist in detoxification processes and may even help curb cravings. For those focusing on bone health, particularly during alcohol recovery, calcium supplements can play a role in addressing bone density loss. However, it’s crucial to consult a healthcare provider before adding any supplements to your routine to ensure they align with your specific health needs.


