Digital tools are transforming addiction recovery. By offering real-time support through apps, wearables, telehealth, and AI chatbots, they address critical gaps in traditional methods. These tools help people manage cravings, track progress, and access support anytime, anywhere. Key highlights include:
- Mobile Apps: Tools like Recovery Connect and A-CHESS provide personalized strategies, location-based alerts, and progress tracking.
- Wearables: Devices monitor stress, cravings, and substance use, sending timely alerts to prevent relapse.
- Telehealth: Remote counseling makes care accessible, especially for those in rural areas or with mobility challenges.
- AI Chatbots: 24/7 support offers coping techniques and crisis intervention during high-risk moments.
- VR Simulations: Immersive experiences build empathy and help families understand addiction triggers.
These tools complement professional care, improving outcomes by bridging gaps between sessions and enabling continuous support. Pairing them with expert guidance ensures a more effective recovery journey.
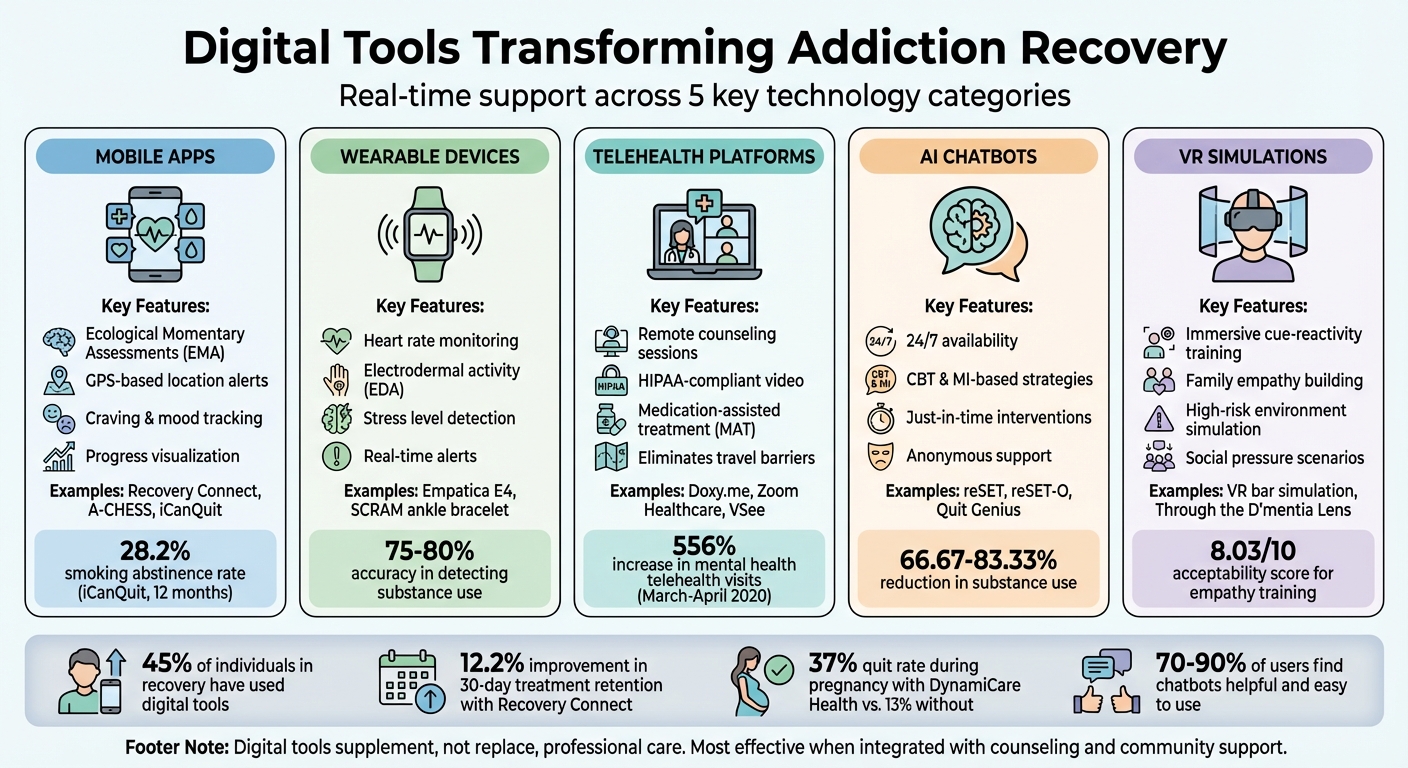
Digital Tools for Addiction Recovery: Features and Examples
Digital Therapeutics in the Treatment of Substance Use Disorders | DEA MATE Act Training Course
sbb-itb-17645e5
Using Mobile Apps for Monitoring and Early Detection
Mobile apps are transforming addiction management by combining Ecological Momentary Assessments (EMA) and passive sensor-based tracking to gather real-time data on substance use, mood, and stress levels. EMA actively prompts users to log cravings and social contexts as they occur. Meanwhile, passive monitoring uses sensors and GPS to automatically collect behavioral data, such as identifying when a person enters a high-risk location like a bar or liquor store.
Biometric tools add another layer of precision by offering objective evidence of use or abstinence. Devices like Bluetooth breathalyzers (e.g., Soberlink, BACtrack) and smartphone-linked carbon monoxide monitors (e.g., iCO Smokerlyzer) provide measurable results. To ensure the data is accurate, some apps incorporate facial recognition or "video selfies" (Video Directly Observed Therapy) to confirm the user is performing the test. A 2024 study highlighted the effectiveness of this approach: participants using DynamiCare Health for remote biometric monitoring achieved a 37% quit rate during late pregnancy and 40% abstinence after delivery, compared to just 13% and 10% for those relying solely on quit line referrals.
The real advantage lies in pattern recognition. Just-In-Time Adaptive Interventions (JITAIs) use data streams like EMA inputs, GPS data, and heart rate to deliver timely, personalized support. Michael S. Businelle from the University of Oklahoma Health Sciences Center explains:
"Substance use and lapse risk in those attempting to quit are dynamic (i.e., they fluctuate over time), idiosyncratic (i.e., they differ between individuals), and driven by multiple factors".
Choosing the Right App for Addiction Management
When selecting an app for addiction management, focus on evidence-based designs, engaging user experiences, and strong privacy protections. Apps grounded in proven therapeutic frameworks like Cognitive Behavioral Therapy (CBT), Acceptance and Commitment Therapy (ACT), or the Community Reinforcement Approach (CRA) tend to deliver better outcomes. For example, a 2020 trial showed the iCanQuit app, based on ACT, achieved a 28.2% smoking abstinence rate over 12 months, outperforming the National Cancer Institute’s QuitGuide app, which achieved 21.1%. Similarly, Zamplo mHealth demonstrated a 45.8% 30-day retention rate in a six-week trial, far surpassing the industry average of 7%.
As Geoffrey Messier from the University of Calgary notes:
"Recovery apps can benefit from flexible designs with customizable degrees of user autonomy".
Privacy is equally essential. The best apps act as private digital journals while offering optional sober living community connections. Pay attention to how the app stores location and health data, and whether it clearly explains its data usage policies. With 45% of individuals in recovery having used an app or website for support at some point in their lives, privacy concerns can significantly influence adoption.
Features to Look for in Addiction-Focused Apps
The right features can make all the difference in managing recovery effectively. Real-time feedback is key. Apps that provide immediate responses to craving trackers or mood logs help users address potential relapses before they occur. Visual tools, like sobriety milestones or instant coping strategies, can also be highly motivating. Research shows that automated digital smoking cessation tools can improve quit rates by 50% compared to self-help methods or no intervention.
GPS-based geofencing is another valuable feature. It sends alerts or support messages when users approach high-risk locations, such as bars or liquor stores. This is especially helpful for those with specific environmental triggers. Apps that allow users to customize their recovery journey, rather than following rigid guidelines, can also reduce overwhelm and improve engagement.
For those seeking advanced functionality, consider apps with biometric verification and medication adherence tracking. Features like Video Directly Observed Therapy or electronic pill reminders ensure continuous support. When choosing such apps, check compatibility with existing devices or assess the affordability of necessary tools. For instance, a SCRAM ankle bracelet costs about $1,500 per device, plus a $5 daily service fee, while CBT4CBT is a more affordable option at roughly $100 when paired with office-based treatments. Free resources like QuitGuide and quitSTART, offered by the CDC and National Cancer Institute, are also worth exploring.
| Feature Type | Functionality | Example Tool |
|---|---|---|
| Biometric | Breath Alcohol Concentration (BrAC) | Soberlink, BACtrack |
| Biometric | Breath Carbon Monoxide (CO) | iCO Smokerlyzer |
| Location-Based | GPS High-Risk Alerts | A-CHESS, Connections |
| Behavioral | Craving & Mood Tracking | reSET, Zamplo |
| Verification | Video Directly Observed Therapy | emocha Mobile Health |
Telehealth and Online Platforms for Remote Counseling
Telehealth has become an essential resource for addiction interventions. During the early months of the pandemic, mental health telehealth visits skyrocketed by 556% between March and April 2020. By April 2023, 68.4% of individuals using telehealth services in the U.S. sought help for mental health conditions. This approach addresses accessibility challenges often found in traditional care settings. Studies comparing in-person and telehealth treatment show no major differences in substance use outcomes, patient retention, or satisfaction. Mariah Bourne, a Community Social Psychologist, emphasizes:
"Research has found online drug and alcohol addiction therapy to be just as effective as in-person therapy".
Telehealth serves as a reliable and secure alternative, complementing on-site care with ongoing support.
Setting Up Telehealth for Addiction Support
To begin, reach out to your insurance provider to find in-network telehealth clinicians. Confirm costs and coverage details with both your insurer and the clinic before scheduling an appointment. Tools like the NIAAA Alcohol Treatment Navigator can help you locate board-certified addiction specialists. These resources allow families to assemble a care team that includes a behavioral health therapist and a physician qualified to provide medication-assisted treatment (MAT).
Ensure the video platform you use is HIPAA-compliant. Platforms like Doxy.me offer a free, secure version with premium upgrades and discounts for non-profits. Other options, such as Zoom, SimplePractice, and VSee, provide features like end-to-end encryption and business associate agreements (BAAs) to meet legal standards. Before your session, test your camera, microphone, and internet connection to avoid technical hiccups. Find a quiet, private spot to maintain confidentiality, and prepare a written list of medications, recent weight, and any questions you have to make the most of your time.
Benefits of Remote Counseling in Addiction Interventions
Once established, telehealth offers numerous advantages. It eliminates geographical barriers, making care accessible to individuals in rural areas, those with mobility challenges, or anyone without reliable transportation. By removing the need for travel, telehealth also saves time and money, allowing patients to focus on recovery while managing work and family obligations, like childcare.
Much like mobile apps and wearables, telehealth extends care beyond traditional settings, enabling immediate, remote interventions. It provides various modes of care, including synchronous (real-time video or phone therapy), asynchronous (sharing medical history for later review), remote monitoring (tracking compliance through tests or video footage), and mobile health apps (offering text-based therapy and daily tracking tools). Additionally, video sessions can give providers a glimpse into a patient’s home environment, offering insights that may not surface in a clinical setting. For sustained recovery, make it a habit to schedule your next follow-up session before concluding your current telehealth appointment.
Wearable Devices for Real-Time Physical Tracking
Wearable technology is adding a whole new layer to addiction interventions, offering continuous monitoring of physical and emotional signals. These devices can track heart rate, skin temperature, and electrodermal activity (EDA), which are key indicators of stress levels. By identifying moments when someone might be at greater risk of cravings or relapse, wearables provide timely insights that can guide intervention strategies.
Take the SCRAM ankle bracelet, for example. It measures alcohol content in sweat every 30 minutes and can detect consumption equivalent to two or more standard drinks. Commonly used in court-ordered monitoring, it’s a reliable tool for tracking alcohol intake. Similarly, wrist-worn devices like the Empatica E4 monitor EDA, heart rate, and movement, achieving an accuracy of 75%–77% through accelerometry. When these metrics are combined, accuracy exceeds 80%.
How Wearables Support Addiction Intervention Strategies
Wearables uncover patterns that might otherwise go unnoticed. For instance, a sudden spike in heart rate or skin conductance can signal heightened risk, prompting Just-in-Time Adaptive Interventions (JITAIs). These interventions deliver immediate support, such as a text with coping tips or an alert to a peer recovery coach. Dr. Stephanie Carreiro, MD, highlights the potential:
"The ability to objectively identify moments of greatest need and to deliver just-in-time targeted interventions would provide a tremendous advantage over the current model of care".
Some wearables integrate GPS geofencing to send notifications when users approach high-risk locations, like a bar or a place where they previously purchased drugs. Others work with contingency management programs, automating rewards for abstinence using sensor data – a more reliable method than relying on self-reports.
Connecting Wearables with Other Digital Tools
The effectiveness of wearables increases when they’re linked to broader digital systems. For instance, syncing wearable data with telehealth platforms allows clinicians to monitor stress and craving trends between sessions, enabling more responsive remote care. Many devices also connect to smartphone apps via Bluetooth, where users can complete Ecological Momentary Assessments (EMAs). These quick surveys capture real-time emotions and contextual data alongside biometric readings.
For optimal results, wrist-worn devices are generally better than chest bands or ankle monitors due to their comfort and higher user compliance. Look for devices with multi-sensor capabilities, combining accelerometry with heart rate and EDA tracking, and ensure compatibility with FDA-authorized apps like reSET or reSET-O, which support evidence-based behavioral therapies. Costs vary, but the SCRAM ankle bracelet is priced around $1,500 per device, with an additional daily service fee of about $5. Transparent policies on data privacy and usage are crucial to building trust and encouraging consistent use. By bridging wearable technology with mobile apps and telehealth, these tools strengthen the hybrid care model, blending digital and in-person support.
Virtual Reality Simulations for Empathy and Understanding
Virtual reality (VR) is changing how families understand addiction by immersing them in lifelike scenarios that mirror the struggles their loved ones face. Through these simulations, families can step into environments like bars or parties that evoke genuine emotional responses. This kind of immersion not only replicates high-risk situations but also helps build empathy between family members.
One way VR achieves this is by recreating detailed, high-risk environments. For instance, researchers Lee et al. developed a "VR bar" simulation in the early 2000s, testing it on 22 participants. The study found that the 3D virtual environment triggered much stronger nicotine cravings and activated pre-frontal cortex activity compared to viewing static 2D images.
Using VR to Build Empathy in Family Interventions
VR’s ability to simulate social pressures and peer dynamics through avatars gives family members a firsthand look at how these interactions can influence drug-seeking behavior. Professor Pasquale Caponnetto from the University of Catania highlights this potential:
"The usefulness of Virtual Reality in the treatment of psychotic disorders derives from the fact that this tool can represent social environments that trigger responses, reactions, and emotions equivalent to what the real world in a given context would create in the mind of patients."
Immersive, first-person experiences also enhance empathy and improve support strategies. Take the "Through the D’mentia Lens" simulation as an example. In a March 2024 study, 35 informal caregivers used this VR program and gave it an acceptability score of 8.03 out of 10. Participants reported significant improvements in their empathy, confidence in offering support, and the quality of their interactions. When applied to addiction interventions, VR simulations that combine environmental cues with social interactions are more effective than those using simple, isolated triggers. By offering real-time emotional insights, VR fits seamlessly into the broader digital intervention landscape, complementing tools like mobile apps and wearables.
Steps for Adding VR to Interventions
For programs looking to incorporate these empathy-building simulations, the following steps can serve as a guide. To maximize the immersive experience, prioritize head-mounted displays (HMDs) over flatscreen options. A 2024 study involving 49 students using the "Anne Frank House" VR app on the Oculus Quest showed that immersive VR significantly enhanced self-reported knowledge, with scores jumping from 3.18 to 4.60. When choosing VR content, focus on programs that highlight cue-reactivity – showing how specific environmental stimuli can trigger cravings.
As you plan implementation, budget for the necessary equipment, such as HMDs, software licenses, and staff training. Ensure your technology infrastructure can handle secure data storage and support graded exposure, starting with neutral scenarios before moving to high-risk environments. Partner with vendors experienced in addiction-related VR content, and verify that all virtual health data complies with regulatory standards. Finally, remember that VR should enhance, not replace, traditional cognitive-behavioral therapy, maintaining the importance of in-person interactions while adding an innovative layer to interventions.
AI Chatbots and Web-Based Programs for Continuous Support
AI chatbots and online platforms are changing the way support is delivered, offering 24/7 assistance during moments of craving or crisis. These tools provide a discreet and anonymous way to seek help, which can ease the stigma often associated with reaching out. Their ability to respond in real time also makes them highly adaptable, paving the way for personalized interventions.
Benefits of AI Chatbots in Addiction Support
AI chatbots, often designed around therapies like Cognitive Behavioral Therapy (CBT) and Motivational Interviewing (MI), provide coping strategies tailored to each user’s stage of recovery. A study in Frontiers in Psychiatry highlighted their effectiveness, reporting reductions in substance use ranging from 66.67% to 83.33%.
What makes these chatbots especially impactful is their ability to deliver "just-in-time" interventions. For example, GPS-based systems can alert users when they approach high-risk areas, while built-in panic buttons connect users to immediate support during distress. Dr. Lisa A. Marsch from Dartmouth College notes:
"Technology-based therapeutic tools have the potential to enable individuals (and optionally an extended support network) to play leading roles in their own care management".
These tools are not only effective but also user-friendly. Studies show that 70% to 90% of participants find them both helpful and easy to use.
Web-Based Programs for Long-Term Recovery
While chatbots excel in providing immediate support, web-based programs are designed to sustain recovery over the long haul. These platforms combine interactive learning, peer support, and expert guidance to create a comprehensive recovery experience.
One example is the Therapeutic Education System (TES), which includes 62 multimedia modules based on the Community Reinforcement Approach. In a multi-site trial led by Dr. Lisa Marsch, TES achieved a 48% abstinence rate compared to 37% for standard treatment. For smoking cessation, the iCanQuit app, which uses Acceptance and Commitment Therapy, outperformed the National Cancer Institute’s QuitGuide in a trial of 2,415 adults, with abstinence rates of 28.2% versus 21.1%.
Peer support platforms like InTheRooms.com also play a crucial role, connecting over 450,000 registered users (as of 2020) through live video meetings, discussion boards, and speaker recordings. These connections help reduce feelings of isolation during recovery. Other programs, such as FDA-authorized tools like reSET and reSET-O, integrate with outpatient care under clinician supervision. Meanwhile, apps like Quit Genius and DynamiCare Health offer direct access to recovery coaches via chat or phone calls.
When choosing a web-based program, it’s essential to look for features like GPS tracking for high-risk situations, HIPAA-compliant data security, and a foundation in evidence-based therapies. These elements ensure the program is both effective and trustworthy.
Using Digital Tools with Sober Living Centers Resources
This section explores how Sober Living Centers’ educational resources work hand-in-hand with digital tools to support recovery. When paired with expert guidance, these tools become even more effective in addressing addiction and promoting recovery. Sober Living Centers provides a wealth of resources that cater to the educational needs of individuals and families navigating the recovery process.
Using Sober Living Centers for Education and Guidance
Sober Living Centers offers educational articles that help users make sense of data from digital monitoring tools. For instance, if a wearable device detects an elevated heart rate or irregular sleep patterns, the resources on the website can help families understand these indicators. Their materials on the causes and symptoms of addiction also equip users with the knowledge to select evidence-based apps and interpret their outputs correctly.
Families can combine the platform’s guides on therapy and prevention with tools like trigger-tracking apps or sobriety clocks. These resources help users align their digital tools with proven recovery strategies. For example, by learning about high-risk situations and relapse triggers on Sober Living Centers, users can set up GPS-based alerts in their apps, creating personalized SOS plans for moments when they feel vulnerable. This integration allows technology to play a more strategic role in recovery.
Combining Digital Tools with Professional Guidance
While digital tools offer real-time support, their true potential is unlocked when combined with professional guidance. According to SAMHSA, Technology-Assisted Care (TAC) is meant to complement, not replace, in-person treatment methods. The most successful recovery plans merge digital monitoring with the professional counseling and community support that Sober Living Centers helps individuals access.
A great example of this hybrid approach comes from Aware Recovery Care. In 2020, they integrated wearable craving-detection devices with wireless breathalyzers as part of their remote care protocols. This approach led to a 17% drop in treatment disruptions over three months, and 88% of the 322 clients reported that remote practices did not compromise the quality of care. This case highlights how thoughtfully implemented digital tools can enhance professional treatment.
Sharing digital data with counselors is another way to improve recovery outcomes. Sober Living Centers encourages this practice, as it allows professionals to develop more tailored recovery plans. Dr. Deena Manion, Chief Clinical Officer at Westwind Recovery, underscores this point:
"These technologies, while promising, are most effective when integrated into holistic treatment plans that include community support and mental health care".
Conclusion
Digital tools are reshaping how addiction interventions are delivered, offering real-time support when it’s needed most. From mobile apps to wearables and telehealth platforms, these tools fill the gaps between in-person sessions and moments of crisis. For example, integrating the Recovery Connect app into clinics led to a 12.2% improvement in 30-day treatment retention among 11,495 patients – a clear indicator of how effective these tools can be.
However, digital tools are meant to supplement, not replace, professional care. As Jorge E. Palacios from Bright Therapeutics explains:
"Technology can play a transformative role in facilitating the entire treatment process and removing barriers to participation".
By combining digital resources with professional guidance, individuals can bridge the gap between counseling sessions, share real-time data with their providers, and access location-based alerts alongside educational tools from platforms like Sober Living Centers.
Key Takeaways for Families and Individuals
If you’re exploring digital tools for addiction recovery, here are some practical tips:
- Opt for evidence-based apps that align with your needs. Look for features like craving and trigger tracking, secure messaging with counselors, and libraries of coping strategies.
- Use GPS tracking tools to help those in early recovery avoid high-risk locations by sending alerts when they approach these areas.
- Pair digital tools with resources from Sober Living Centers to better interpret data from monitoring apps and make more informed decisions about treatment options.
- Share app data with counselors to help them create personalized strategies based on your real-time patterns and triggers.
- Acknowledge the growing preference for digital tools. Research highlights strong patient interest in smartphone-based interventions as part of their recovery journey.
Digital tools enable continuous support during critical moments, but their real power lies in being part of a broader recovery plan. When technology works hand-in-hand with professional care, recovery becomes a more seamless and ongoing process, offering hope and structure to those on their journey.
FAQs
How do I know if an addiction app is evidence-based?
To determine if an addiction app is grounded in science, look for evidence of validation through peer-reviewed studies or clinical trials that confirm its effectiveness. Apps regulated by organizations like the FDA or backed by published research addressing substance use disorders are typically more trustworthy. Always examine the app’s research thoroughly to ensure it aligns with established scientific standards before relying on it for treatment.
Are telehealth addiction sessions private and HIPAA-compliant?
Telehealth addiction sessions are private and meet HIPAA compliance standards when conducted on platforms specifically designed for this purpose. These platforms use secure, encrypted communication to safeguard patient confidentiality and ensure privacy.
What should I do if a wearable or app flags a high relapse risk?
If a wearable device or app warns of a high relapse risk, it might be a good time to explore digital tools that offer real-time support. These tools can help tackle challenges like stress or cravings as they arise. It’s also wise to involve your healthcare provider or addiction specialist – they can help interpret the alert and make necessary adjustments to your treatment plan. Digital therapeutics can work alongside other therapies, offering additional support to better manage the chances of relapse.